Sciatica refers to pain radiating along the course of the sciatic nerve, which runs from the lower back to the buttock, to the back of the thigh and into the lower leg and the foot (Figure 1). Sciatica usually affects one side of the body. The largest number of cases involving sciatica are due to disc herniations. Sciatica is not a diagnosis! It is a symptom of an underlying condition.

Piriformis syndrome is a condition that may cause sciatica. The piriformis muscle could be compressing the sciatic nerve (Figure 2).

The condition of sciatica due to compression by a herniated disc is called lumbar radiculopathy.
Piriformis syndrome is a condition that causes sciatic nerve symptoms due to compression of the sciatic nerve around the buttock and the hip. The condition is usually connected to the piriformis muscle and its relationship to the sciatic nerve. The piriformis muscle runs from the sacrum to the hip and it is within close proximity to the sciatic nerve (Figure 3). The sciatic nerve exits below and anterior to the piriformis muscle.

What causes piriformis syndrome?
The relationship of the sciatic nerve passing beneath the piriformis muscle may cause the syndrome. Piriformis syndrome may also be caused by anatomical anomalies such as a split piriformis muscle (Figure 4), vascular structures, and variation of the sciatic nerve path.

Piriformis syndrome may also be caused by tightness, adhesions or spasm of the piriformis muscle that will press on the sciatic nerve. This is usually caused by overuse activities such as bicycling and other sporting activities. This pressure being placed on the nerve will cause swelling, inflammation and symptoms of nerve irritation (Figure 5).
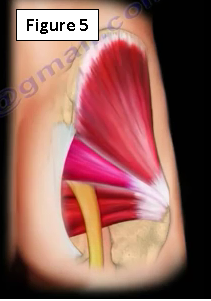
Clinical Diagnosis of Piriformis Syndrome
The most common presentation is pain in the posterior gluteal region and buttock that shoots down the leg in the area of the sciatic nerve that causes symptom-like sciatica (Figure 6). There will be symptoms of burning, tingling and shooting pain, especially when sitting.
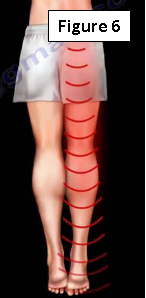
Provocative Tests
Fair Test — flexion, adduction and internal rotation of the hip that will reproduce the symptoms due to the tension of the piriformis muscle (Figure 7).

Lasegue’s Test — the straight leg raising pain is aggravated by forced ankle dorsiflexion (Figure 8).

Piriformis syndrome needs to be differentiated from true sciatica! Both could have the same symptoms, however they each have different causes. The diagnosis should be done by excluding possible spine problems that could be compressing the spinal nerve root and causing sciatica.
The main cause of a true sciatica is a lumbar disc herniation. When the patient complains of sciatica-related pain, the doctor needs to ask themselves a question: is this sciatica due to compression on the sciatic nerve itself? Or, is it due to compression on the roots of the sciatic nerve? Get a MRI to rule out the spine as a cause of compression on the nerve roots of the sciatic nerve (Figure 9). If the patient does not have a herniated disc but has symptoms of sciatica, then the patient probably has piriformis syndrome. The physician can feel the tenderness over the piriformis.

Treatment
Conservative treatment includes; anti-inflammatory medication, physical therapy and stretching of the piriformis muscle, and injection (ultrasound guided or under fluoroscopy). Make sure that the patient has someone present to drive them home, because the sciatic nerve may become numb leaving the patient unable to drive.
Surgery is a last resort and includes the release of the piriformis muscle and sciatic nerve neurolysis. Surgery is done after the physician excludes any possible spine conditions and after the patient has a positive test from injection of the piriformis muscle (they must acknowledge that they feel better after the injection). Piriformis syndrome is probably a diagnosis of exclusion!
For more information on sciatica and piriformis syndrome, follow the links below:
Sciatica, Disc Herniation and Piriformis Syndrome
For more information on various topics, visit my YouTube Channel:
Originally published at www.huffingtonpost.com on March 6, 2017.

